We provided a detailed explanation of what gluten is, what it does in the body, as well as its main sources.
This article is for people who are (or suspect they are) gluten sensitive or intolerant. We will dive into the effects gluten has on our health and what we can do to heal our gut, alleviate symptoms and optimise our immune system.
What triggers Celiac disease later in life?
Celiac disease is an autoimmune disorder that primarily affects the small intestine. People with Celiac disease experience an immune reaction when eating gluten.
Epi means "above" and this is to show that there is something more powerful than genetics. Put very simply, our genetics determines what we are susceptible to, and likely to develop, but how we live our life determines whether these susceptibilities actually come to fruition.
Put another way, genetics loads the gun and our environment pulls the trigger.
Not all that long ago it was thought that our genetics determined our health, that it was all a matter of chance. After spending $300 million and mapping the human genome, it was found that there weren’t as many genes as was once thought. It turned out that more important than our Genetics was the concept of Epigenetics.
So, what are these things that pull the trigger on Celiac disease?
- gut issues
- gut infections
- overburdened by stress
- immune issues
- exposure to Glyphosate from the weed killer RoundUp
- mold exposure
- constant exposure to gluten and cross-reactive foods
What can mimic Celiac disease?
Celiac disease is an Autoimmune condition that affects the intestines. Due to this, there are a lot of conditions that can mimic Celiac disease, including;
- Intestinal Hyperpermeability (aka Leaky gut)
- Inflammatory bowel disease (IBD)
- Hashimoto’s Thyroid disease
- Adrenal insufficiency
- Microscopic colitis
- Crohn’s disease

These conditions can have similar presentations and they are also likely to occur alongside Celiac disease. This is due to Celiac disease being an autoimmune condition, leading to inflammation and damage to the intestines which will impact many other bodily systems as a flow on effect.
Can you be gluten sensitive and not celiac?
Many will say they are gluten sensitive, as they don’t feel right after eating gluten. And tests will come back negative for Celiac disease.
Many diagnosed with Celiac are told there is no such thing as gluten sensitivity, you either have Celiac disease or you don’t. This causes some with Celiac to get annoyed or even scoff their noses at those who claim they’re gluten sensitive, as they feel it lowers the validity of their disease.
There is not an on and off switch with the harms from gluten. It is not a simple binary yes or no, you have harm or you don’t. Even those with Celiac disease can vary in the severity of their illness.
Celiac disease or not, gluten is known to increase levels of zonulin, which is a marker of intestinal hyperpermeability. Thus, people with pre-existing gut issues or even just genetic susceptibilities to gut issues are more likely to be sensitive to gluten.

Many will often note that when they are feeling robust and healthy they are able to handle gluten without any issues while when they’re already not feeling the best, the effects of gluten are exaggerated.
What does Celiac stool look like?
It usually has 4 legs, a seat and a supported back.
Terrible dad joke, I know.
The stool of a person with Celiac Disease can vary per person, though here is the general picture.
- It is often looser than usual, a bit more watery and tending to the diarrhea side of things.
- After gluten exposure some can also have bleeding of their intestinal tract which can show up in the stool as redness or even a darker than usual colour to the stool.
- There can also be signs of fat malabsorption which presents as pale coloured stool, that can leave a greasy layer on top of the toilet bowl and an overall foul smell.
- Due to the issues with digestion, it is also possible that the stool has more undigested foods than an otherwise healthy person.
What is the difference between IBS and gluten intolerance?
IBS is short for Irritable bowel syndrome and its symptoms include:
- Bloating and gas
- Constipation and/or diarrhea
- Cramping
- Abdominal pain
Given that it is a syndrome, there is no test to diagnose it, but it is instead a diagnosis of exclusion, meaning that other diseases are ruled out first. On that same vein, given that it is a syndrome, there can be many possible causative factors that contribute to the imbalance which causes IBS to manifest.

Clinical overlap between IBS and IBS-like disorders.
Image source: www.researchgate.net
Interestingly, all of these symptoms can also occur in gluten sensitivity as well. It is possible that gluten exposure can contribute to the development of IBS and studies have found a link between the two. That is not to say that all IBS is due to gluten in the diet, though, given its ability to impair intestinal function and lead to leaky gut, it is certainly an intervention to consider early on.
Can you suddenly become gluten intolerant?
Yes.
As we mentioned above, the study of Epigenetics says that we are not relegated to the genetic lottery. Certainly our genetics play a role in determining what we’re susceptible to, yet our overall health, lifestyle and environment determines
Some people are genetically susceptible to gluten intolerance or Celiac disease and are fine their whole life, up until they’re not fine.
There is a concept known as the allostatic load which is your overall body burden of factors that can contribute to ill health. When we reach a certain threshold, disease begins to manifest, and in those with susceptibilities to Celiac disease, immune issues and gut issues they may show up as the inability to have a healthy respond to gluten now or permanently. This is analogous to Death by a Thousand Cuts.
How do you know if you are allergic to gluten?
There are many tests that can be performed to determine how your body responds to gluten.
On the more invasive side of things is a biopsy of the small intestine. This is done via an endoscopy, where a camera views your small intestine and a tissue sample is taken, to be analysed. This is thought to be the most accurate measure of whether someone has Celiac disease.
Can a blood test detect gluten intolerance?
There is a simple blood test for Celiac disease to look for antibodies. The downside of this test is that you have to be on a diet containing gluten for it to accurately pick this up, not great if somebody feels horrible on gluten. Though in that scenario, you probably don’t need a test to tell you that gluten is an issue for you.
What other tests can let me know about gluten intolerance?
There are genetic tests which can determine your likelihood of having issues with gluten, though won’t say whether you do or do not. The genes in particular are HLA-DQ2 and HLA-DQ8. Companies such as 23andMe sequence certain parts of your genome for you. The genes they test for are updated periodically so it is worth checking just what genes are being tested for.
Though not a test specifically for gluten allergies, intestinal hyperpermeability tests can determine how ‘leaky’ your gut lining is, which would necessitate removing foods that lead to ‘leakiness’, such as gluten.
How do I know if I am gluten or dairy intolerant?
Dairy intolerance is usually quite an easy one as the effects can happen quite rapidly.
After having a decent serving of lactose from dairy containing foods, one or all of the following may occur within a couple of hours or less.
- Bloating
- Gas
- Diarrhoea
- Stomach cramping
You’ll note these are very similar symptoms to gluten intolerance.
There is a difference between a dairy allergy and dairy intolerance. With a dairy allergy, any amount of dairy, no matter how minute, can trigger a response. However, with an intolerance, it is the dose that makes the poison, so to speak. Intolerances to dairy come from underproduction of the enzyme lactase in our intestines. Thankfully, supplementing with the enzyme lactase can reduce or completely eliminate the symptoms by enabling us to digest lactose properly.
The simple at home test is to cut them both out of your diet, reintroduce one, gauge your symptoms. Cut them both out again, add the other one, gauge your symptoms and see how you go.
There is also a possibility that on their own neither leads to any issue but the combination does. This could indicate that both are causing some degree of harm to your body and is just unnoticeable on its own.
Can you test for gluten intolerance at home?
Yes and no.
As mentioned above, eliminating then reintroducing gluten containing foods and gauging symptoms can be done from the comfort of your own home, but isn’t always the most accurate way to check.
Checking for your genetic susceptibilities can be done from home, via a saliva test from 23andMe, though again, this doesn’t diagnose anything.
For a blood test or biopsy to get a more accurate representation, you’re going to have to leave the house.
How do I know if I'm gluten intolerant or wheat intolerance?
Another simple at home test. If you notice issues from eating wheat based foods and don’t notice any issues from gluten-containing grains such as spelt or rye, it could be the wheat and not the gluten that is an issue.
This can get muddied as you are very rarely eating just wheat or any of the other gluten-containing grains in isolation.

Source: Mayo Clinic
What happens to your body when you stop eating gluten?
As mentioned above, gluten leads to intestinal permeability, damage to the intestines, an over-activated immune system, inflammation and all the issues that stem from that. By avoiding gluten (and other substances that harm your health), you begin to healing process as your body is no longer constantly bombarded with the offending factors.
Expect to see things such as:
- Reduction in inflammation as measured by symptoms such less pain, puffiness, water retention & fat retention. Or simply on a blood test.
- Improvement in digestive health and less digestive symptoms
- Less signs of nutrient deficiencies as you’re able to absorb more nutrients from your foods
- Increased energy
- Much more
If you’re on the severe end with Celiac you’ll likely notice some drastic changes, particularly if you’re somehow who has been eating gluten your whole life, though fully repairing the damage to the intestines can take a lot of work depending on the severity of it.
What relieves gluten pain?
Abstaining is the best way to relieve gluten pain in the long term. Alongside targeted protocols for the gut and immune system which we’ll mention below.
However, exposure is going to affect a lot of people, whether that be intentional or accidental from a well-meaning family member (especially the ones making Freekeh salads thinking it’s gluten free).
As mentioned above, supplementing with a gluten digesting enzyme around the meals you suspect you have been or will be exposed is a great way to reduce the incidences of a gluten attack. These enzymes are by no means going to be a solution for those with Celiac disease, especially considering just how little gluten is needed to trigger an attack in those with Celiac disease.
Taking a good quality digestive enzyme supplement can also assist, as the gut as a whole will be compromised. If the gut is struggling to digest other foods this will just add to the overall burden experienced from the gluten issue.
Magnesium can be a great mineral to supplement with. The reason for this is that gluten can really bring on pain, cause stress for the body and cause spasm of the digestive system. Stress depletes magnesium, magnesium helps us handle pain and is also needed to relax spasming of the digestive system.
Activated charcoal can be a remedy to quickly assist with any gas and intestinal issues caused by gluten ingestion. And indeed other irritants to the gut.
Other anti-inflammatories like turmeric and ginger may also assist in the healing process.
Malabsorption
Additionally, given that the intestines and overall digestive function is heavily compromised in those with Celiac disease, it’s important to address the issue of malabsorption.
Years ago the mantra was, "you are what you eat". More recently, in an age of digestive issues, that’s been altered, "you are what you absorb".
This is why eating the perfect diet is no longer enough, we have to address how well our body is actually digesting and assimilating these nutrients.
For those really struggling to boost up levels of certain nutrients due to digestive issues, there are some workarounds to consider.
Intravenous injection of nutrients has become a lot more accessible in recent times and is a fantastic way to bypass the digestive system and give your body a boost to replete levels of certain nutrients.
If that ain’t your cup of tea, then there are also some supplements:
Liposomal supplements get absorbed through the mucous membranes without the need for digestion, then into the bloodstream and right into the cell much more readily than non-liposomal supplements that still need to get through to the intestines.
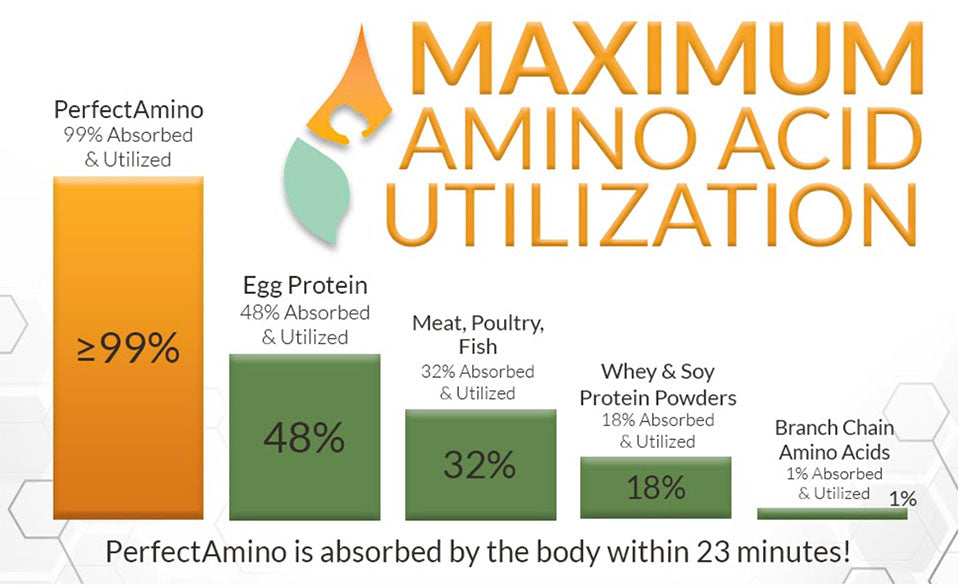
Unfortunately, there aren’t liposomes available for every nutrient and this is where a highly bioavailable form of the nutrient can come in handy. We all know the benefits of protein and it is even more important when digestive issues are present as protein is needed for building and repairing damaged areas of the body.
PerfectAminos contains amino acids in a specific ratio to enhance the bioavailability of it, meaning you’re absorbing much more than you would with other supplements like whey protein and even wholefood sources:
How do you fix gluten intolerance?
The issues with gluten intolerance come about from gluten’s effect on our intestines and the subsequent immune overactivation and inflammation. Our intestines and bloodstream are separated by a barrier that is one cell thick with mucous protection.
As mentioned above, 3 important factors involved in improving your tolerance for gluten containing foods are:
- healing the gut
- reducing inflammation
- modulating the immune system
To improve this, abstinence from gluten and cross reactive substances for the duration of the protocol is imperative. Additionally, black pepper, alcohol and chilli are all known to increase gut permeability and may be helpful to avoid during this healing period.
To improve the health of the digestive tract, there are many things to consider, which could be a whole article in and of itself, here are just some factors to scratch the surface.
Read more: Top 5 Tips to Improve Gut Health Naturally
How we eat matters
Our body digests optimally when we’re in a relaxed state. When we eat at our office chair and don’t have a distinct break between work and our meal, our body doesn’t have enough time to enter a parasympathetic nervous system state (the rest and digest branch of our autonomic nervous system). This is the balance to our sympathetic nervous system, known as our fight, flight, freeze branch.
What we eat matters
A wholefoods based diet is a great start, yet everybody also has their own nuances. What is medicine for me right now may be hindering you. We have to consider our own bio-individuality. This is where testing and working with a practitioner can be quite handy. But beyond all that, developing self awareness will help.
How we digest matters
In instances where we aren’t producing enough digestive juices to meet our demands, digestive enzyme supplementation can be quite beneficial.
The health of the organisms in our gut matters
With the spotlight on the microbiome, probiotics have hit the mainstream in a big way the past 10+ years. But they’re not all created equally and neither are we. Certain strains have different effects within the body and are more likely to be beneficial if there is a deficiency in those strains.
A strain that helped out your friend may or may not help you. And while we’ve been focused a lot on the bacteria living inside us, there’s also the mycobiome to consider, the ecosystem of fungi which can also influence how well we respond to our diet and environment.
Whilst scientific researchers and practitioners alike are looking at the best ways to determine which probiotics are best for which individual sometimes experimentation can be a great solution. A targeted formula for addressing leaky gut may be just the product you need.
How else can we heal the gut and immune system?
Aloe vera juice is one such remedy used by herbalists for many years. Aloe vera has demulcent properties given by its sticky internal juices. This demulcent quality provides a bandaid-like effect to the gut, speeding up healing.
Additionally, immune system overactivation from gluten exposure can be remedied by things such as medicinal mushrooms. Reishi is particularly beneficial at modulating the immune system.
Put simply, modulating is the act of bringing the system more to balance. If it’s overactive, it can calm the system. If it’s underactive, it can boost the system. These herbs/plants have intelligence that they confer onto humans.
These are just scratching the surface on some ways to assist with healing the gut and immune system though are by no means a comprehensive strategy on their own.
How do I detox my body from gluten?
Gluten isn’t something we would classically think of as needing to detoxify. Levels don’t build up in the body like plastics and heavy metals. However, the effects of gluten can build up and get worse with continuous exposure.
The best way to "detoxify" from the effects of gluten is to firstly eliminate exposure and secondly to repair the damage it has caused.
Gluten proteins are resistant to breakdown by proteolytic enzymes in the gastrointestinal tract. Normally, they just past through us undigested without incident. But us gluten sensitive folks are not so lucky. In case of acute exposure, having some DPP-IV containing enzymes can break down gluten to reduce the harmful effects on your system. Other than that, becoming aware of which wholefoods and processed foods contain gluten.
To heal the damage, check out the advice in the above section as well as working with a practitioner well-versed in gut and immune conditions.
Glu(ten)ing it all together
As we can see, gluten is not something that affects just a small portion of the population. Whether you have Celiac disease, gluten sensitivity or not, gluten is going to be affecting your intestines and immune system to varying degrees.
Thankfully, there are many gluten-free options available and products we can keep on hand for accidental or conscious exposure to gluten and many therapies, herbs, supplements and more to help us improve any damage caused by this mischievous little protein.
Order BiOptimizers in Australia at OptimOZ: Cognibiotics, Masszymes, P3-OM, HCL Breakthrough, Gluten Guardian, Power Flush, Parasite Guardian, Magnesium Breakthrough, Kapex and Leaky Gut Guardian
References:
1. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3945755
2. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5587842
3. https://www.sciencedirect.com/science/article/abs/pii/S0016508513001352




Share:
What Is Gluten and What Does It Do in the Body?
Biohacking Digestion and Optimising Gut Health